Surgery, Anaesthesia and Perioperative Medicine
This information is for you and your family if you are coming to our hospital for surgery. We want to help you feel confident about your surgery.
At Prince of Wales Hospital we perform these types of surgery:
- Cardiothoracic – heart and lung surgery
- Ophthalmology – eye surgery
- Orthopaedics – bone and joint surgery
- Plastic Surgery – repair or reconstruct skin or other body tissue
- Neurosurgery – nerve, spinal cord or brain surgery
- Vascular surgery – surgery on arteries or veins
- Urology – surgery on the urinary system including bladder and kidneys
- General surgery including: upper gastrointestinal tract, colorectal, oncology surgery
- Dental, oral and maxillofacial - teeth, jaw and face surgery
- Ear, nose and throat surgery.
The information below will help you plan and prepare for your surgery. We provide information on what to expect before, during and after your surgery.
How we can help you

Waiting for surgery

Preparing for surgery

The day before surgery
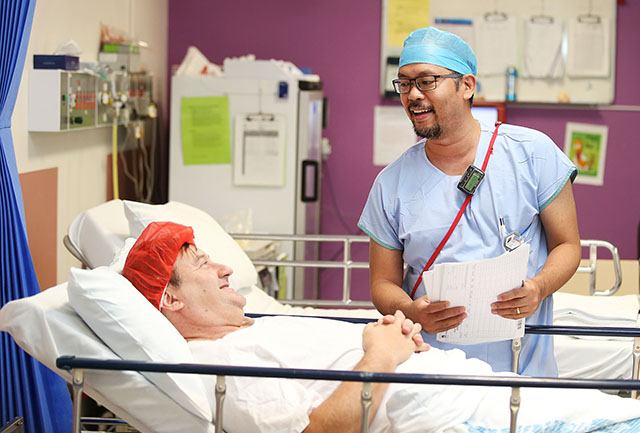
The day of your surgery
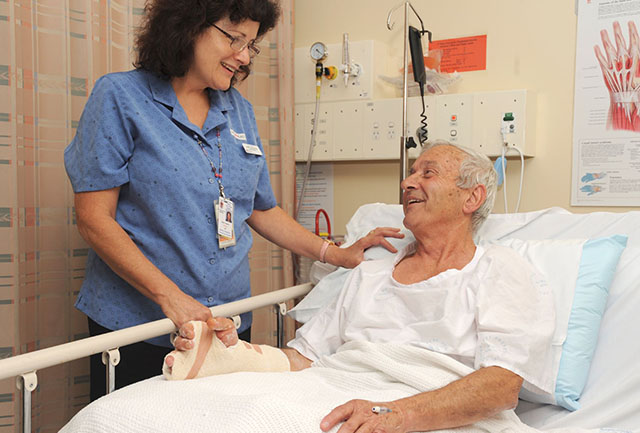
After your surgery

Going home
